Radiology
Radiotherapy (commonly known as electrotherapy) is a method of treating cancer. It works by using ionizing radiation to control or destroy malignant cells to treat patients.

Radiation therapy uses high-energy radiation to kill or destroy tumor cells and prevent them from continuing to grow, divide, or spread. Cancer radiation therapy is a localized treatment, typically affecting only the irradiated area of the body, and is suitable for treating breast cancer, head and neck cancer, lung cancer, esophageal cancer, colorectal cancer, etc. Radiation planning and precision in Hong Kong have significantly improved, and damage and side effects on surrounding benign cells have been greatly reduced.
For inquiries about the cost of cancer radiation therapy, please contact reVIVE Oncology and Cancer Centre.

Applicable cancers
- Mammary Cancer
- Colorectal (intestinal) Cancer
- Oesophageal Cancer
- Head and Neck Cancer
- Lung Cancer
- Prostate Cancer
- Brain Tumour
Side effects of radiotherapy
- Redness and stinging of skin within the treatment area
- Fatigue
- Nausea and vomiting
- Diarrhoea
- Hair Loss
- Headache
- Difficulty in Swallowing
- Stiff Joints and Cramping
- Soft Tissue Fibrosis
- Sexual Dysfunction

Post-electrotherapy Care
- Maintain skin care within the treatment area, avoid sun exposure and wear loose clothing.
- Get enough rest and sleep.
- Eat small meals and avoid fried, spicy, sweet, and oily foods.
- Wear a suitable wig, headgear, or hat.
- Steroids or painkillers that lowered brain pressure can be taken to alleviate headaches.
- Appropriate exercise and massage can improve joint stiffness and cramping.
Volumetric Modulated Arc Therapy, VMAT
The effectiveness and precision of radiation therapy are closely related, as it aims to kill cancer cells while minimizing the impact on normal cells. Our center is equipped with the most advanced radiotherapy equipment. Here are some introductions:
Volume-controlled arc radiotherapy is a volume-intensity-controlled rotational radiotherapy technique. During the 360-degree rotation of the linear accelerator gantry, doctors use image guidance to precisely optimize the gantry speed, dose rate, and multi-leaf collimator, and a sophisticated computer system to concentrate the dose as much as possible on the tumor area. Currently, this therapy is recognized as an effective treatment for various cancers, including intracranial, head and neck, prostate, and cervical tumors.
Compared to traditional therapies, VMAT significantly reduces treatment time by 50-80%, which effectively decreases the time patients with unstable conditions (such as unstable breathing) spend in the treatment room, lowering the risk of emergencies.
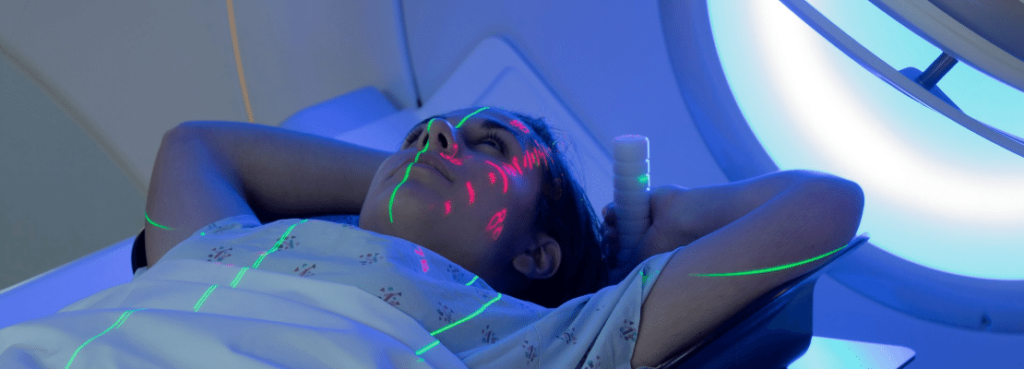
Active Breathing Coordinator™
Due to respiratory factors causing tumor movement, the Active Breathing Coordinator system helps patients hold their breath and control lung capacity during simulation and radiation therapy, thereby reducing body movement and enhancing accuracy while significantly decreasing the radiation dose received by surrounding vital organs or normal cells.
The entire process of the Active Breathing Coordinator system is governed by strict protocols: before undergoing breathing-controlled radiation therapy, the medical team will create a personalized mold for the patient to connect with the breathing control device, perform CT simulation, and carry out treatment planning and dose calculations. After the treatment plan is confirmed by the doctor, precise breathing-controlled radiation therapy is executed.
Adaptive Radiation Therapy
During radiation therapy, patients may experience loss of appetite, leading to weight loss and changes in body shape and facial contours.
Adaptive radiotherapy can record the patient's outline and confirm it through computer scans. Doctors can then accurately determine the appropriate treatment. With clear images, doctors can observe the patient's daily condition and quantify the tumor's response during radiotherapy, thereby adjusting the treatment plan according to changes in the tumor.
Helical Radiation Therapy
Helical radiation therapy is an advanced treatment system that integrates treatment planning, positioning, and intensity-modulated radiation therapy (IMRT) functions. It accurately delineates the area requiring radiation therapy, calculates optimal beam distribution and dosage, tracks changes in tumor shape and position, and focuses the beams on the tumor while minimizing damage and side effects to surrounding tissues.
Precisely combats cancer cells
Generally speaking, when the tumor has spread widely and in a scattered manner, radiotherapy is not recommended to avoid excessive side effects.
The unique spiral radiotherapy system utilizes a 360-degree photon incident angle and synchronous movement of the treatment bed, and features a spiral intensity-modulated radiation therapy (IMRT) technology with up to 51 angles. This accurately identifies the areas requiring radiation therapy, avoids normal tissue, and focuses on attacking cancer cells. Combined with a 3D computer-aided treatment planning system, an adaptive image-guided radiotherapy (IGRT) system, a precise patient positioning system, and a quality assurance system, it forms a complete treatment system, thus providing patients with an efficient and safe treatment option.
For patients with multiple lumps throughout the body or those requiring extensive irradiation, the spiral radiotherapy technique can cover an area of up to 160 centimeters, thus shortening the treatment time to a single session.
Accurately locates the tissues
The patient's position during each treatment session cannot be exactly the same, and the movement of tumors and organs within the body can introduce discrepancies. Therefore, before each treatment, it is necessary to obtain images of all tissue positions using the built-in CT of the equipment and compare them with the original treatment plan images to identify and immediately correct any relevant three-dimensional spatial discrepancies, ensuring precise targeting of the tissue during treatment.
Although this process takes one to four times longer than traditional treatments, it helps understand changes in tumor size, records the cumulative dose to the tumor and surrounding tissues for personalized dose adjustments, and accurately calculates dose distribution to protect normal tissues and avoid unnecessary side effects.
Stereotactic Radiation Therapy
Stereotactic radiation therapy is a highly precise form of radiation therapy that uses special tools to fix the patient's position, ensuring accurate irradiation and reducing damage to surrounding tissues. It is primarily used for treating tumors in the head and neck region.
Stereotactic radiotherapy (SRS) uses high doses of radiation to completely destroy tumors in several sessions, requiring less time compared to traditional low-dose radiotherapy. It provides a safe and effective treatment for elderly patients or those with severe conditions who are not suitable for conventional treatment.
Before starting stereotactic radiation therapy, doctors utilize helical radiation therapy technology (TomoTherapy) to observe real-time images of the patient's body, determining the precise location of the tumor. The helical radiation therapy technology can simultaneously address multiple tumor locations, greatly saving time. Additionally, using Radionics' fixation devices helps lock in the tumor's position while minimizing the impact on normal tissues.
Image-Guided Intensity-Modulated Radiation Therapy
Image-guided technology enhances the precision of radiological diagnosis and treatment, ensuring accuracy in every treatment session.
Intensity-Modulated Radiation Therapy
Intensity-modulated radiation therapy (IMRT) uses numerous fine beams from different angles that converge at the cancer site, concentrating high doses on the tumor while reducing damage to normal tissues. It adjusts the radiation dose distribution based on the tumor's shape and the relevant positions of surrounding tissues.
Image-Guided Technology
Image-guided technology enhances the precision of radiation therapy. Since a patient's position can vary with each treatment, and tumors and organs continuously move, it is essential to obtain images of all tissue positions using orthogonal two-dimensional X-ray images or CT scans before each treatment. These images are then compared with the original treatment plan images to identify and correct any discrepancies.
Three-Dimensional Conformal Radiation Therapy (3DCRT)
Three-dimensional conformal radiation therapy (3DCRT) inputs information from CT scans into the treatment planning system, reconstructing the tumor shape and designing a dose distribution that conforms to its outline, delivering an evenly distributed dose from various entry angles. However, this technique still has room for improvement. Some tumors may exhibit concave or C-shaped distributions, such as nasopharyngeal tumors often encasing the cervical spine, raising concerns about excessive radiation exposure to the spinal cord. Normal tissues like the parotid gland may also receive higher doses, making complications difficult to avoid. IMRT can be considered an enhanced version of 3DCRT, as it optimally distributes radiation intensity based on each patient's individual circumstances using advanced software for treatment design.
Operation of Intensity-Modulated Radiation Therapy
When establishing a treatment plan, in addition to the shapes of the tumor and normal tissues, factors such as maximum tolerable doses must also be inputted. The computer calculates the necessary parameters for treatment, and a tumor specialist selects feasible methods, which is known as "inverse planning." Tumors and other tissues can be divided into multiple small units, with the dose each point receives composed of beams from multiple small areas at various angles.
Superficial Radiation Therapy
Surface radiotherapy can effectively treat common skin cancers, including basal cell carcinoma, squamous cell carcinoma, and Karposi's sarcoma.
The treatment utilizes low-energy X-rays, ranging from 50 to 150 kV. These X-rays penetrate only moderately to the skin's surface, minimizing damage to deeper tissues and effectively preventing scarring. Furthermore, for cases with a high risk of postoperative recurrence, additional surface radiotherapy after surgery can significantly improve the overall cure rate.
Prone Breast Radiation Therapy
In traditional treatments, breast cancer patients would receive therapy in a supine position. However, the current prone breast therapy allows patients to lie face down during treatment, letting the treated breast hang away from the chest wall, thereby reducing the exposure of lung and heart tissues and other normal tissues to radiation.
Dose distribution images show that lung tissues of patients receiving prone therapy are exposed to significantly lower radiation than those receiving supine therapy. Furthermore, larger-breasted women benefit more from the prone position, resulting in higher treatment efficacy.
A study of 245 women diagnosed with early-stage breast cancer found that the prone position was acceptable to most patients during breast radiotherapy, with only a few (approximately 4.9%) reporting pain in the chest wall or ribs; none of the patients requested a mid-section rest. This position ensures an even distribution of radiation throughout the breast, minimizing the dose received at the top and bottom. The prone position can be considered a more effective posture for treating breast cancer.
Remote High-Dose Afterloading Brachytherapy
This treatment involves delivering radiation therapy to the tumor surface using a radiation source (Ir192) at close range within a cavity or space, concentrating high-dose radiation on the tumor while minimizing damage to surrounding tissues and organs.
Suitable cases for Brachytherapy include:
- Cervical cancer, uterine cancer and vaginal cancer
- Breast cancer brachytherapy
- Boost in nasopharyngeal carcinoma treatment
- Suitable wigs, wigs, or hats can be worn.
- Neck cancer recurrence and re-treatment
- Intraluminal boost in oesophagal cancer treatment, etc.
For inquiries about the information and cost of radiotherapy, please contact reVIVE Oncology and Cancer Centre.
Hotline
-
Telephone Inquiry
New customer inquiry: 3001 5810
Existing customers: 2156 5838 -
WhatsApp inquiry
3001 5810 -
E-mail
enquiry@reviveonco.com.hk -
Opening Hours
Mon-Fri: 9:30am - 6:30pm
Sat: 9:30am - 1:30pm
Closed on Sundays and Hong Kong public holidays -
Mong Kok Clinic
12/F, Office Tower, Langham Place, 8 Argyle Street, Mong Kok, Kowloon
Fax: 3579 0153
EC Specialists Premium (PHF No.: DP000104)




